Overview
In this section you will find methods and tools you can use for development, implementation and evaluation of care pathways. Although there are many quality improvement tools (e.g. flowcharts, Ishikawa diagram, 5 times why et cetera) already published, we present a number of tools and methods developed specifically for care pathway projects. Each tool or method is discussed briefly, illustrated with an example, and a reference to a paper with background information is provided.
This section starts with the 7-phase method for development, implementation and evaluation of care pathways, as this provides the framework for the other tools.
7-phase method for development, implementation and evaluation of care pathways
The 7-phase method was developed by an international team of researchers, clinicians and managers, to support multidisciplinary teams in the development, implementation, evaluation and continuous monitoring of care pathways. It can be used in different health care settings, within and across organizations.
The method consists of seven consecutive phases, although it is always possible to return to a previous phase. It should serve as a guideline to support teams when developing and implementing care pathways.
Each of the seven phases has a specific contribution to the development, implementation and monitoring of a well-organized care process, but it is the combined action between the phases which forms a whole, greater than the sum of its parts.
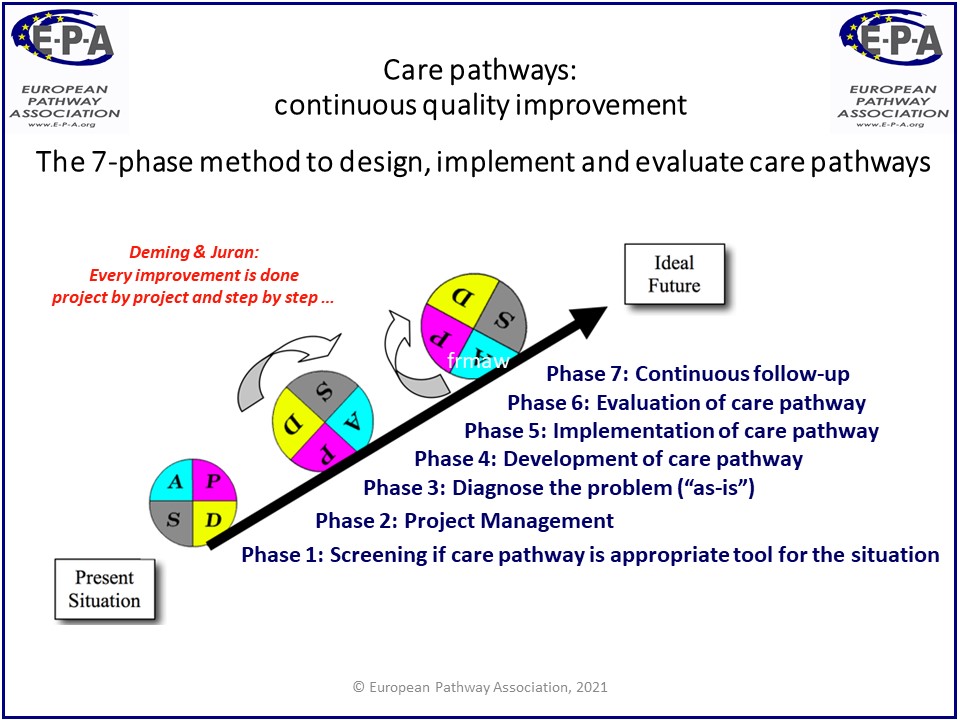
1) Screening phase – is a care pathway the right tool for the problem we need to solve; who will be the owner of the project / care pathway?
2) Project management phase – do we have the right people, time, budget to start a project; what are our goals?
3) Diagnostic and objectification phase – what is our current practice? Based on four perspectives: own organization & team, vision of patient & family, available evidence & legislation, and external partners
4) Development phase – design and development of the care pathway, based on input from previous phases.
5) Implementation phase – piloting and adjusting the care pathway, followed by implementation for daily use
6) Evaluation phase – evaluation of the care pathway: effect, usability and compliance to the care pathway
7) Continuous follow-up phase – keeping the pathway alive by monitoring, adjusting the pathway
Vanhaecht, K., Van Gerven, E., Deneckere, S., Lodewijckx, C., Janssen, I., Van Zelm, R., … & Sermeus, W. (2012). The 7-phase method to design, implement and evaluate care pathways. International Journal of Person Centered Medicine, 2(3), 341-351.
The table below gives an overview of which tools are typically used in which phase.
| 1. Screening | 3-blackboard method; CPSET* |
| 2. Project management | Gantt chart |
| 3. Diagnosis | 3-blackboard method; CP Compass; CPSET; Importance Performance Analysis |
| 4. Development | Gantt chart |
| 5. Implementation | Implementation model |
| 6. Evaluation | Importance Performance Analysis |
| 7. Follow-up | CP Compass |
The Leuven Clinical Pathway Compass
Although developed almost 20 years ago, the Leuven Clinical Pathway Compass is still a valuable conceptual framework to help in measuring the impact of care pathways. The Compass is based on existing measurement tools, including the well-known Balanced Score Card, the Value Compass, and the DataMap. The Leuven Clinical Pathway Compass consists of five domains of indicators.
These domains can be used at patient group level to evaluate the impact of a care pathway. The domains are:
- Clinical, containing clinical and functional indicators, both pathway specific (e.g. time to bowel function is a colorectal surgery pathway) as well as generic (e.g. pain scores)
- Service, containing indicators which can be used to evaluate the service of the care pathway team (e.g. patient satisfaction and/or experience of the cere process)
- Team, describing indicators that can be used to assess the impact on teamwork (e.g. job satisfaction, relational coordination) – it can be a difficult domain to evaluate because care pathway teams are not necessarily delivered by well-defined teams
- Process, containing the indicators to evaluate the process of care delivery (e.g. process lead times, waiting times, sequencing of activities, compliance)
- Financial, including the indicators which can be used to assess the financial impact of a care pathway (e.g. number of tests, time spent, length of stay).

The figure above shows the Compass with some examples of indicators per domain. Not all domains are relevant for every care pathway project. It is up to the team to decide which indicators to measure and follow-up, based on the goals of the project. The Compass can also serve as a framework to discuss and formulate the goals of a care pathway project, by systematically looking at all five domains. For some indicators, the domain is debatable. For example length of stay can be explained as a proxy for cost, while at the same time it provides information on process and service. The added value of the Compass is to evaluate the care process from different perspectives.
Vanhaecht, K., & Sermeus, W. (2003). The Leuven clinical pathway compass. Journal of Integrated Care Pathways, 7(1), 2-7.
Conceiving the ‘ideal’ care pathway – the 3-blackboard method
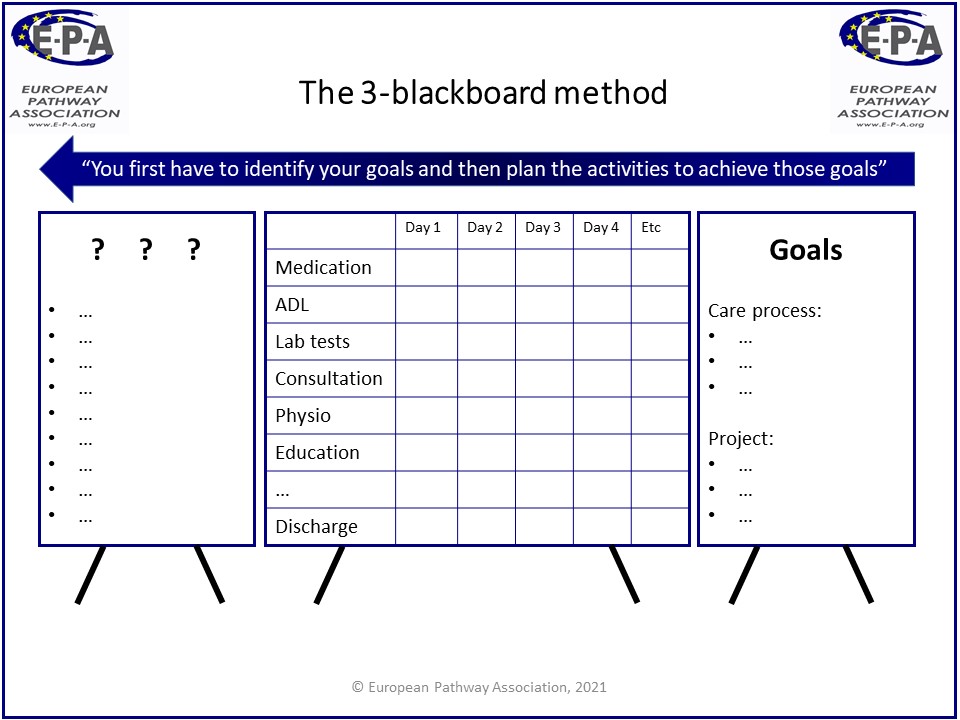
The 3-blackboard method is a consensus building technique for explicating the clinical content of a care pathway. The method was first developed at the Center for Case Management (CCM) in Boston (www.cfcm.com). The method was further elaborated within the Belgian Dutch Clinical Pathway Network and E-P-A master classes, and is used in the ‘screening phase’ of the 7-phase model. The method is based on the slogan: “you first have to identify your goals, and then plan the activities to achieve those goals!”
Getting started
The 3-blackboard method can be used in phase 1 (as a structured brainstorm), but is predominatly used in phase 3, as a method to elaborate the perspective of the organization and team. The method is used by the CP development team during a project meeting. Participants should have real-life experience with the care process. Based on our experience, we suggest a group of 7–12 participants for this session. Make sure there are actually three blackboards (or white boards, or flip charts, …) available.
Right hand board: goals
The first step is to discuss and define the specific goals. These are documented on the right hand board, signaling that this is what the team works towards. Goals are defined on two levels:
(1) The care process: goals at the level of the patient group. Usually these goals comprise the discharge or transfer criteria for the patient
(2) The project: these are targets the team (or the organization) tries to achieve with the development and implementation of the CP. For this level, the domains from the Leuven Clinical Pathway Compass can be used.
Middle board: time-task matrix
The middle board contains the activities that should be included in the CP in a later stage. It is a common pitfall to try to reach too much detail in the activities at this stage. During the 3 blackboard session, the activities should be restricted to the so called key interventions. Usually the middle board is formatted as a time-task matrix, where each row represents a category of specific actions, and each column a moment in time. Sometimes different formats are useful, such a goal-task matrix, time-discipline matrix, or a flow chart.
Left hand board: bottlenecks and question marks
The final board is used to write down any points of discussion, bottlenecks, questions et cetera that arise during the session. This way, the discussion on the clinical content can continue, while making sure important questions, discussion points and other items are documented. These items have to be cleared up or objectified in a later stage during the project.
Next steps
After the 3-blackboard session, there remain several important steps in the development of the CP. Obviously, the middle board has to be filled in with details. Next, based on the 3-blackboard method, the Diagnosis-phase of the seven-phase model can be executed in order to objectify the content from the three boards.
Vanhaecht, K., Van Zelm, R., Van Gerven, E., Sermeus, W., Bower, K., Panella, M., & Deneckere, S. (2011). The 3-blackboard method as consensus-development exercise for building care pathways. International Journal of Care Pathways, 15(2), 49-52
The Gantt chart to describe the ideal care pathway
A Gantt chart is a tool typically associated with project management. It is a specific kind of horizontal bar chart which visualizes a project planning. Another common name for the Gantt chart is the time-task matrix. As early as 1991, Karen Zander from the Center for Case Management, Boston, published on the use of Gantt charts to visualize a care pathway.
The basic form of a Gantt chart or time-task matrix is very straightforward. In project management, each row represents a project activity. The columns represent the timeframe for the project. The project manager decides which activities are executed in which period, depicting this in the appropriate rows of the chart. This way, the Gantt chart provides a visual project planning and overview. In this form, a Gantt chart is a valuable tool in the phase 2 of the 7-phase method: project management.
In addition, during the development phase of the 7-phase method, the same format and principles can be used used: the activities (daily care, lab tests, medications, treatments, diet, et cetera) each fill a row. The columns represent the timeframe, see the example below or the example in the 3-blackboard method.

Specific forms
There are several variations possible from this basic form. A first variation can be the ‘time- discipline’ or ‘time-profession’ matrix. In this case, each involved discipline or profession fills a row in the Gantt chart. This can be a helpful tool to determine the overlap in activities by different disciplines. A second variation is the ‘goal-task’ matrix where the timeline is formed not by calendar time, but by goals that have to be met before the patient can proceed in the care pathway.
Other variations in the timeline are possible. Sometimes the day-by-day format is useful, in more longer term care pathways a week-by-week, month-by-month or phased (screening, diagnosis, treatment, rehabilitation, …) format is more suitable. In emergency care, an hour-by-hour format might be useful. Also the location where the care is delivered can be used to represent the timeline, resulting in the ‘location-task’ matrix. Here each column represents a physical location (e.g. emergency department, operating theater, nursing department) in the order in which the care process usually flows.
Not all care pathway are visualized as Gantt charts. For example if the flow of a care processes is not predictable in a timeline, a flowchart or decision tree can be a good alternative to visualize the process.
Zander, K. (1991). Care maps: the core of cost/quality care. New Definition, 6, 1-3.
Care Process Self-Evaluation Tool
The Care Process Self-Evaluation Tool (CPSET) was developed and validated in 2007. The tool assesses key characteristics of care processes/care pathways that impact the organization of these processes. It is a self-evaluation tool: the scores are based on the perceptions of (multidisciplinary) team members involved in the process. This self-evaluation can be used as input in phase 1 and 3 of the 7-phase method. It shows how the different members perceive the actual organization of the care process relative to each other, allowing for meaningful discussion on the important characteristics.
The five key characteristics of well-organized care processes which are assessed with the CPSET are:
1) coordination of the care process
2) patient-focused organization
3) communication with patients and family
4) collaboration with primary care
5) follow-up of the care process.
The CPSET consists of 29 items, arranged in these five key characteristics. The items are operationalized in 10-point Likert scales (totally disagree (1) to totally agree (10)). An average score per key characteristic (or subscale) can be calculated and visualized, e.g. in a radar plot.
The figure below shows two examples (fictitious data) of radar plots based on CPSET scores. In this example, a number of medical doctors, allied health professionals and nurses assessed a care process. The radar plot on the left shows the scores of the individual nurses, whereas the radar plot on the right shows the average scores per involved discipline. The figure shows that the scores per subscale vary. For example, nurse 6 scores relatively low on patient-focused organization (PFO). And the average score of the MD’s is higher in comparisson with the other disciplines on communication with patients and familiy (COM). Discussing these data with the team can reveal why a score from an individual or discipline might be different from other scores. Rather than trying to reach consensus on the subscales, the goal should be to explore the different visions of the team members.

PFO = patient-focused organization; COR = coordination of the care process; COM = communication with patients and family; CPC = collaboration with primary care; FU = follow-up of the care process
Vanhaecht, K., De Witte, K., Depreitere, R., Van Zelm, R., De Bleser, L., Proost, K., & Sermeus, W. (2007). Development and validation of a care process self-evaluation tool. Health Services Management Research, 20(3), 189-202.
Seys, D., Deneckere, S., Sermeus, W., Van Gerven, E., Panella, M., Bruyneel, L., … & Vanhaecht, K. (2013). The Care Process Self-Evaluation Tool: a valid and reliable instrument for measuring care process organization of health care teams. BMC health services research, 13(1), 1-7.
Importance-Performance-Analysis: setting improvement priorities in care pathway development and implementation
Care pathways are tools to coordinate and organize care processes. All care pathways consist of multiple interventions, and combine the clinical perspective (optimal care) with the management perspective (optimal organization of care). The use of care pathways can generate insight in several challenges that healthcare teams face in practice:
Management challenges:
- Providing objective data / feedback on current process
- Variation between patients and between hospitals
- Optimal utilization of resources
- Setting priorities for quality improvement
Research challenges:
- Dealing with different levels of evidence for interventions
- Putting evidence into practice
- Identification of key interventions and quality indicators
- Setting priorities
An Importance-Performance-Analysis (IPA) helps to set the improvement priorities for multi professional teams working with care pathways. This post shows the concept of IPA, illustrated with results from care pathway research projects on COPD and colorectal cancer surgery, supported by the European Pathway Association.
In an IPA, all interventions which are listed in the care pathway are mapped in a matrix. The importance dimension of each intervention is showed on the Y-axis. In the COPD study the Y-axis was based on international guidelines and validated by an expert panel. This resulted in a continuous range from 0 – 100%. In the colorectal cancer study, the importance was defined by the strength of the recommendation of each intervention based on the international ERAS® protocol, ranging from 1-5.
The performance dimension, on the X-axis, is defined by the adherence rate: in which percentage of patients is the intervention actually performed? This results in a 2-by-2 matrix, in which each intervention from the care pathway is represented by a dot. The top-right quadrant shows interventions that are important and have a high adherence. The bottom-left quadrant shows interventions that are less important with a low adherence. This could be interventions with an individual indication for specific patients. The bottom-right quadrant shows interventions with high adherence, but low importance. This could be overtreatment, but this can also be new interventions with a low level of evidence because research is still in progress. The top-left quadrant shows the ‘room for improvement’: these are interventions that are important, but have a low adherence.

Importance-Performance-Analysis provides an intuitive way to visualize ‘missed care’, and helps in making teams aware of their performance and room for improvement. Setting the cut-off points in IPA can be challenging; in the colorectal surgery study, a 70% cut-off was based on previous studies, showing increased patient outcomes with adherence rates ≥70%. The other cut-off points are based on discussion, and can be somewhat arbitrary.
This text is based on a poster presentation at the International Conference on Integrated Care 2019 (Van Zelm et al., 2019).
Seys, D., Bruyneel, L., Decramer, M., Lodewijckx, C., Panella, M., Sermeus, W., … & Vanhaecht, K. (2017). An international study of adherence to guidelines for patients hospitalised with a COPD exacerbation. COPD: Journal of Chronic Obstructive Pulmonary Disease, 14(2), 156-163.
Van Zelm, R., Sermeus, W., Coeckelberghs, E., Seys, D., Panella, M., & Vanhaecht, K. (2019). Setting improvement priorities: Importance-Performance-Analysis in care pathways for integrated care. International Journal of Integrated Care, 19(4).
Van Zelm, R., Coeckelberghs, E., Sermeus, W., van Overstraeten, A. D. B., Weimann, A., Seys, D., … & Vanhaecht, K. (2017). Variation in care for surgical patients with colorectal cancer: protocol adherence in 12 European hospitals. International journal of colorectal disease, 32(10), 1471-1478.
